 A complication of heparin therapy may be heparin-induced thrombocytopenia, which is defined as a sudden decrease in platelet count by at least 30% of baseline levels. The principal complication of anticoagulant therapy is spontaneous bleeding, and it can be detected by microscopic examination of urine. The following complications should be monitored and managed: 
Encourage early mobilization and leg exercises to keep the blood circulating adequately. Intermittent pneumatic compression devices increase blood velocity beyond that produced by the stockings. Compression stockings prevent dislodgement of the thrombus. In some cases, signs and symptoms of a pulmonary embolus are the first indication of DVT.ĭeep vein thrombosis can be prevented, especially if patients who are considered high risk are identified and preventive measures are instituted without delay. Tenderness, which usually occurs later, is produced by inflammation of the vein wall and can be detected by gently palpating the affected extremity. Also called massive iliofemoral venous thrombosis, the entire extremity becomes massively swollen, tense, painful, and cool to the touch. 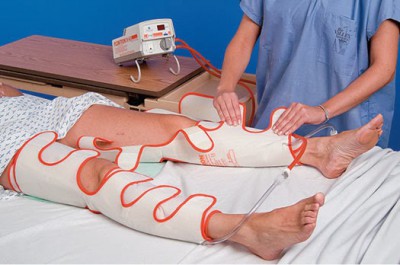
With obstruction of the deep veins comes edema and swelling of the extremity because the outflow of venous blood is inhibited Repetitive motions may cause irritation to the vessel wall, causing inflammation and subsequent thrombosis.Ī major problem associated with recognizing DVT is that the signs and symptoms are nonspecific. Normal pregnancy is accompanied by an increase in clotting factors that may not return to baseline until longer than 8 weeks postpartum, increasing the risk of thrombosis. Oral contraceptives use also lead to hypercoagulability. Increased blood coagulability occurs most commonly in patients for whom anticoagulant medications have been abruptly withdrawn. Direct trauma to the vessels, as with fracture or dislocation, diseases of the veins, and chemical irritation of the veins from IV medications and solutions, can damage the veins. The exact cause of deep vein thrombosis remains unknown, but there are factors that may aggravate it further. It is estimated that as many as 30% of patients hospitalized with DVT develop long-term post-thrombotic complications.The incidence of DVT is 10% to 20% in general medical patients, 20% to 50% in patients who have had stroke, and up to 80% in critically ill patients.The incidences of deep vein thrombosis that occurs together with pulmonary embolism are: After an acute episode of DVT, recanalization or reestablishment of the lumen of the vessel typically occurs. 
Fragmentation of the thrombus can occur spontaneously as it dissolves naturally, or it can occur with an elevated venous pressure. The “tail” can grow or can propagate in the direction of the blood flow as successive layers of the thrombus form. Venous thrombi are aggregates of platelets attached to the vein wall that have a tail-like appendage containing fibrin, white blood cells, and many red blood cells. Formation of a thrombus frequently accompanies phlebitis, which is an inflammation of the vein walls. Damage to the intimal lining of blood vessels creates a site for clot formation. Venous stasis occurs when blood flow is reduced, when veins are dilated, and when skeletal muscle contraction is reduced.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
